Mead Family Dental
3630 Shattuck Rd. Saginaw, MI
Hours
Monday: 8am-1pm, 2pm-5pm
Tuesday: 8am-1pm, 2pm-5pm
Wednesday: 8am-1pm, 2pm-5pm
Thursday: 7am-2pm
Blog Posts
The Clock is Ticking
The Halloween decorations are still up, but not for too much longer. It's still about ghosts and goblins for now, but soon it's going to be more about turkey and stuffing. I hear this noise. [...]
The true cost of a crown
I recommend a crown or an onlay to lots of my patients. It's one of the most common procedures we do and we do it very well if I say so myself. A crown is created [...]
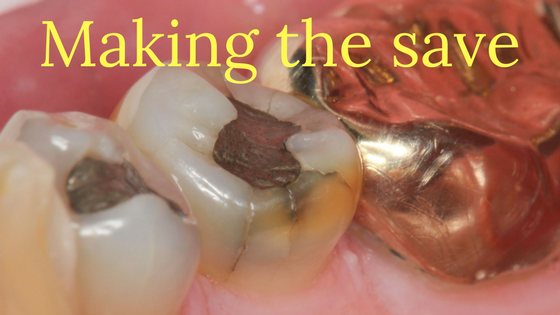
Making the save
Last week I found myself in a spot that I don't like to be in. A couple of times. I found myself preparing a crown on a tooth that was in much worse shape than I [...]
Gum disease doesn’t cause heart disease
Contrary to what you hear from a LOT of dental marketing, heart disease isn't caused by gum disease. It's technically correct that gum disease and heart disease are correlated or "linked," but there is currently no evidence [...]
April 15,2022
Pay Online with our “Patient Portal”
Our “Patient Portal”, located under the “Forms” button, will allow new and existing patients to sign up and access account info, treatment info, upcoming appointment info, the ability to pay online plus more! Sign up and check it out!
We’re Back!
Friday May 29th, 2020
We’re baaaack! Whoo Hoo!
The carpets are clean our filters are changed some new barriers are up and our attitudes are 100% ready to go back to work!

What has changed?
In order to keep our patients and team safe, we’ll be screening patients when they arrive. What’s that going to look like?
Your temperature will be checked
We’ll ask you some health screening questions, verbally. But don’t worry…it’s an easy test. We’ll give you the questions in advance!
Have you, or anyone close to you, experienced flu-like symptoms within the past 14 days such as:
Cough: Yes / No
Fever: Yes / No
Shortness of Breath: Yes / No
Sore Throat: Yes / No
Muscle/Body Aches: Yes / No
Nausea/Vomiting: Yes / No
Fatigue: Yes / No
A recent lack of taste or smell: Yes / No
Have you come into contact with anyone who has tested positive for COVID-19? Yes / No, If yes, when________
Have you been tested for COVID-19, Yes / No
If yes, was it a positive or negative result? Positive / Negative
See…nothing to it! One other thing, we’d ask you to check your temperature at home before your appointment if you can. If you have a fever, call the office and we’ll figure out what’s next!
Changes in scheduling and protocols:
You’ll notice some other changes in scheduling and protocols to help keep everyone safe. For instance, we’ve staggered our appointment times. Upon your arrival there should only be one other patient waiting, if any. If you prefer to wait in your car, please check in first. You can call us at (989) 799-9133) and we can let you know when we’re ready for you!
In an effort to keep the fewest number of people at the office, we ask that you come alone, if able. If you have someone accompanying adult patients, they will need to wait outside.
Existing appointments with Dr. Mead for treatment:
If you have a scheduled appointment with Dr. Mead for treatment, it is still on the schedule and we’ll be expecting you! You will NOT receive a text for the next few weeks. (Texts have been disabled until the schedule is up to date.)
We will contact you ASAP to confirm your appointment with the date and time. Each appointment is key to catching up with our patients who have been waiting to see us. With that said, a 48 hour notice is required to change or cancel any scheduled appointment. You may leave a message on the machine, email us at: alanmeadoffice@gmail.com, or call us during normal business hours (989)799-9133.
A $25.00 “no show” fee will be enforced for patients who miss scheduled appointments.
Existing appointments dental hygiene visits:
If you have a scheduled appointment with our hygienist for teeth cleaning, most appointments will still be on the schedule and we will be expecting you. You will NOT receive a text for the next few weeks. (Texts have been disabled until the schedule is up to date.)
We will contact you ASAP to confirm your appointment with the date and time. Each appointment is key to catching up with our patients who have been waiting to see us. With that said, a 48 hour notice is required to change or cancel any scheduled appointment. You may leave a message on the machine, email us at: alanmeadoffice@gmail.com, or call us during normal business hours (989)799-9133.
A $25.00 “no show” fee will be enforced for patients who miss scheduled appointments.
EXCEPTION!! If you have a scheduled appointment on a Tuesday with the hygienist we may have to change your cleaning appointment.
Why? Our amazing dental hygiene team of Shannon and Tanna is now just the very amazing Shannon! For the moment our Tuesdays will only have one hygienist working, so we might have to re-arrange some appointments for a little while. Don’t worry, though! We’ll catch up!
I want to schedule an appointment
Existing patients: We would prefer an email at alanmeadoffice@gmail.com. Include your full name, reason for appointment, and contact info. We will contact you as soon as possible. You can call the office at (989) 799-9133 as well. We expect to be a bit swamped for the next few weeks so if you get the answering machine please leave a message and we’ll get back to you ASAP!
New patients: We can’t wait to meet you! Ideally you would send us an email at alanmeadoffice@gmail.com. Include your full name, reason for appointment, and contact info. We will contact you as soon as possible. You can call the office at (989) 799-9133 as well. WE LOVE NEW PATIENTS and we think you’re going to love our office, but we’re currently doing our best to catch up with the high demand! So please be patient with us!
For any other questions…please email us at alanmeadoffice@gmail.com!
We can’t wait to see you and get back to “normal!”
Dr. Alan Mead and team
Welcome!
My name is Dr. Alan Mead, and for over 20 years my staff and I have provided patients with a different, fun, experience at our dentist office in Saginaw, MI.

IT’S WHAT WE DO
COSMETIC DENTISTRY * WHITENING * FILLINGS * CROWNS
* ROOT CANALS * BRIDGES * PARTIALS * IMPLANT RESTORATIONS
* BITE GUARDS * EXTRACTIONS * CLEANINGS * PERIO MAINTENANCE * EXAMS * X-RAYS * CONSULTS
Our Primary goal is to provide everyone with remarkable dental care in the very best dental office setting imaginable.
Don’t let the laid back and comfortable atmosphere fool you though, this office is serious about your dental health!

Ready? Let’s do this!
If you haven’t already given us your information, bring your dental insurance card with you. If you have Delta Dental you may not have a card but…most Delta Dental plans provide a website we can access to get a real time status of your benefits. Most other insurance companies do not.
Inform us of any dental visits you’ve had within the last 12 months. Include treatment from oral surgeons, specialists, out of town emergencies, or any other treatment that would have been charged to your dental insurance. Your remaining insurance benefits are what we use to calculate the estimates.
If you require an estimate, as to the out of pocket cost for your first visit, please allow an estimated 2 weeks to receive the information back from your dental insurance provider.
All intake forms and necessary information needed for your first visit is located on our “Forms” page.
Once your appointment is scheduled you will receive a text.
If you are unable to keep your scheduled appointment, a 48-hour notice by text, email, answering machine or call is required to avoid a $50.00 missed appointment fee.
IT’S ALL ABOUT YOU!!!!..and us
We want you to be comfortable and presented with all information needed to understand and improve your dental health and making your smile everything you have wished for. When your teeth are healthy and looking spectacular… you’ll be happy and we’ll be happy.
Win, Win!
Seldom does “I’ll just wait until it hurts” work with dental concerns. If you’ve put off coming in, we will not judge or overwhelm you with hard to understand dental lingo.
We will, however, present you with a treatment plan that is explained, and deemed necessary, by Dr. Mead. You also have the choice of seeing what Dr. Mead sees with an overhead view of your exam in progress! After that, it’s up to you how we proceed.
Ready to schedule that first appointment?
GREAT! Contact our office and we’ll take it from there.
Insurance
Dental insurance is confusing. In network, out of network, 100% means 80%, fee schedules, waiting periods, predeterminations, deductibles, blah, blah, blah.
Bottom line: you want to know how much will it cost out of your pocket!
We can do that.
Mead Family Dental participates, and is “in network”, with Delta Dental insurance as a Premier participating provider.
(excluding: Delta Dental Healthy Michigan and Healthy Kids)
If your dental insurance plan accepts claims from “out of network” providers,
we will be happy to submit your dental claims for you.
Mead Family Dental is considered “out of network” with the exception
of Delta Dental Premier plans.
The following insurance plans do not accept dental claims from
“out of network” providers:
Delta Dental Healthy Michigan
Delta Dental Healthy Kids
Medicaid
Meridian
Molina

Check if your dental insurance plan accepts claims from “out of network” providers.
SURPRISE!
You owe more than expected!
Not good, right?
To avoid an unwanted surprise, be sure to ask that a pre-determination of treatments be sent to your dental insurance company.
Note: Dental predeterminations are an estimate of benefits not a guarantee of payment. Check in with our office,
before your appointment, to confirm an approved estimation of benefits has been received. If it becomes necessary to unexpectedly change treatment during your procedure, Dr. Mead will inform you before proceeding.
We will do our best to provide you with a new estimate.
Note: We will submit dental claims, on your behalf, but you are responsible for all unpaid balances.
No dental insurance? No problem. Check out our Gold Club section.
“GOLD CLUB”
We are pleased to offer the Mead Family Dental “Gold Club”
to our patients without dental benefits.
Our goal is to help you have the beautiful, healthy smile that you want and deserve.
There are many reasons why some people stay away from the dentist, but one comment
we hear frequently is “I couldn’t come because I didn’t have dental insurance.”
Enrollment fee is $305.00 (for a 12 month period)
Additional adult, in same household, $210.00 ea.
Additional child, under the age of 14 and in same household, $190.00 ea.
Included for the enrollee/s:
*Two regular adult or child prophys (equal to $164.00)
Full set of x-rays (equal to $130.00)
Yearly oral cancer exam and
one emergency exam (equal to $55.00-$137.00)
20% discount on all treatment done within our office
20% even applies to elective procedures such as whitening and veneers!
Payment is due at time of treatment
Credit cards accepted with the exception of Care Credit.
NOTE: All prices listed below are subject
to change without notice
Gold Club savings breakdown
Regular prophy (cleaning) adult: $82.00 (two included with Gold Club)
Child Prophy (cleaning) under 14 yrs old $72.00 (two included with Gold Club)
*Difficult prophy (full mouth debridement) $210.00 (uses both Gold Club cleanings)
Fluoride $45.00 ($36.00 out of pocket with Gold Club) $9 savings
4 Bitewing x-rays $58.00 (all included with Gold Club)
1 Periapical x-ray $32.00 (all included with Gold Club)
1 Panoramic x-ray $130.00 (all included with Gold Club)*Initial exam (new patient) $82.00 (included with Gold Club)
Emergency exam *$82.00 (one included with Gold Club)
Periodic oral exam *$55.00 (one included with Gold Club)
A total of two exams per 12 months with Gold Club
Restorations
Resin- one surface filling $172.00 ($137.00 out of pocket with Gold Club) $35 savings
Resin- two surface filling $198.00 ($158.00 out of pocket with Gold Club) $40 savings
Resin- three surface filling $235.00 ($188.00 out of pocket with Gold Club) $47 savings
Resin- four surface filling $325.00 ($260.00 out of pocket with Gold Club) $65 savings
3 unit bridge $3155.00 ($2524.00 out of pocket with Gold Club) $631 savings
Crown $1040.00 ($832.00 out of pocket with Gold Club) $208 savings
Partials, Extractions
Partials $1,420.00 ($1,136.00 out of pocket with Gold Club) $284 savings
Extractions (simple) $155.00 ($124.00 out of pocket with Gold Club) $31 savings
Extractions (surgical) $270.00 ($216.00 out of pocket with Gold Club) $54 savings
Whitening $360.00 ($288.00 out of pocket with Gold Club) $72 savings
Perio maintenance prices with Gold Club
$30.00 out of pocket for each of the first two perio maintenance cleanings
$140.00 out of pocket for the 3rd perio maintenance cleaning, if done within the 12 month Gold Club window.
You will pay $200.00 total, out of pocket, for 3 perio maintenance visits.
Note: Without Gold Club, total would be $525.00. You save $325.00.
*Gold Club “FINE PRINT” details:
All family members start date is the same as initial enrollee
Payment in full is due on day of treatment
Cash, Check, Credit/Debit cards accepted with the exception of CareCredit
No refunds
Payments
Payment Options
Paying for your treatment is manageable at Mead Family Dental.
We accept Cash, Checks, Visa, MasterCard, Discover,
AMEX, Debit and CareCredit.
20-3-Free* option for amounts totaling over $1,000.00
You’ll need 20% down
Then make 3 equal payments monthly on remaining balance
Free of added administration fees
*With approved credit card on file*
Pay Online with our “Patient Portal”
Our “Patient Portal”, located under the “Forms” button, will allow new and existing patients to sign up, access account info, treatment info, upcoming appointment info, the ability to pay online plus more! Sign up, with this secure site, and check it out! (Security clearance may take up to 2 weeks)


Text Us
(989) 267-8938
Be sure to add your name in your text and add us into your contacts.

AlanMeadOffice @gmail.com
We will read and respond. Promise.

Fax: (989) 497-8110
We don’t expect many of these.